9 Hidden Signs of Diabetes You Should Never Ignore
You may not notice diabetes all at once. It tends to develop quietly, with small changes that slowly become part of your routine.
A little more thirst. Slight fatigue. Minor shifts that feel easy to ignore. At some point, you might pause and ask yourself, how do I know if I have diabetes or how do you know if you have diabetes before it becomes serious?
That question deserves attention. The signs and symptoms of diabetes often reflect deeper metabolic imbalance involving insulin function, glucose regulation, and long-term cellular stress.
According to the International Diabetes Federation, hundreds of millions of people worldwide live with diabetes, and many are unaware of it.
If you want clarity on how to know if you have diabetes, the body usually provides signals. The key lies in recognizing patterns early and responding with intention.
9 Hidden Signs of Diabetes
The nine unexpected symptoms that could signal diabetes are a collection of metabolic, neurological, and immunological responses to high blood glucose, each pointing to the body’s struggle to function without proper glucose regulation.
These signs are often the first clues that something is amiss, appearing long before more severe complications arise. They are less obvious than extreme thirst or urination but are direct consequences of the same underlying problem.
1. Unexplained Weight Loss: This occurs primarily in Type 1 diabetes but can also happen in advanced Type 2. Without enough insulin to help glucose enter the cells for energy, the body starts burning fat and muscle for fuel. This breakdown of tissues leads to a noticeable drop in weight even if you are eating normally or more than usual. The body is essentially starving at a cellular level, forcing it to consume its own reserves.
2. Increased Hunger (Polyphagia): Despite eating, you may feel constantly hungry. This is because the body’s cells are not getting the glucose they need for energy due to insulin resistance or lack of insulin. This lack of cellular energy triggers hunger signals, creating a vicious cycle where you eat more, but the glucose still can’t be used effectively, leading to even higher blood sugar levels.
3. Frequent Infections: High blood sugar levels can weaken the immune system, reducing the body’s ability to fight off bacteria and viruses. This can lead to more frequent infections, such as skin infections, urinary tract infections (UTIs), and gum disease. Hyperglycemia creates an environment where bacteria can thrive, and it also impairs the function of white blood cells that are crucial for fighting pathogens.
4. Slow-Healing Sores or Cuts: Elevated glucose levels damage nerves and impair circulation, particularly in the extremities like the feet. Poor blood flow means that nutrients and oxygen needed for tissue repair cannot reach the wound site efficiently. This, combined with a weakened immune response, dramatically slows down the healing process, turning minor cuts or sores into persistent problems that are prone to infection.
5. Blurred Vision: High blood sugar can cause the lens of the eye to swell, which changes its shape and ability to focus, resulting in blurry vision. This effect is often temporary and can fluctuate as blood sugar levels go up and down. However, if left unmanaged over the long term, hyperglycemia can damage the blood vessels in the retina (diabetic retinopathy), leading to permanent vision loss.
6. Tingling, Pain, or Numbness in Hands or Feet (Neuropathy): This is one of the most common complications. Excess sugar in the blood is toxic to nerve fibers, especially the long nerves that extend to your hands and feet. This damage, known as diabetic neuropathy, can interfere with nerve signals, causing symptoms that range from tingling and burning sensations to complete numbness.
7. Recurring Yeast Infections: Yeast (Candida) feeds on sugar. High glucose levels in the blood translate to higher sugar levels in bodily secretions. This creates a favorable environment for yeast to overgrow, leading to frequent infections in both men and women. These can manifest as genital yeast infections, oral thrush, or fungal infections on the skin.
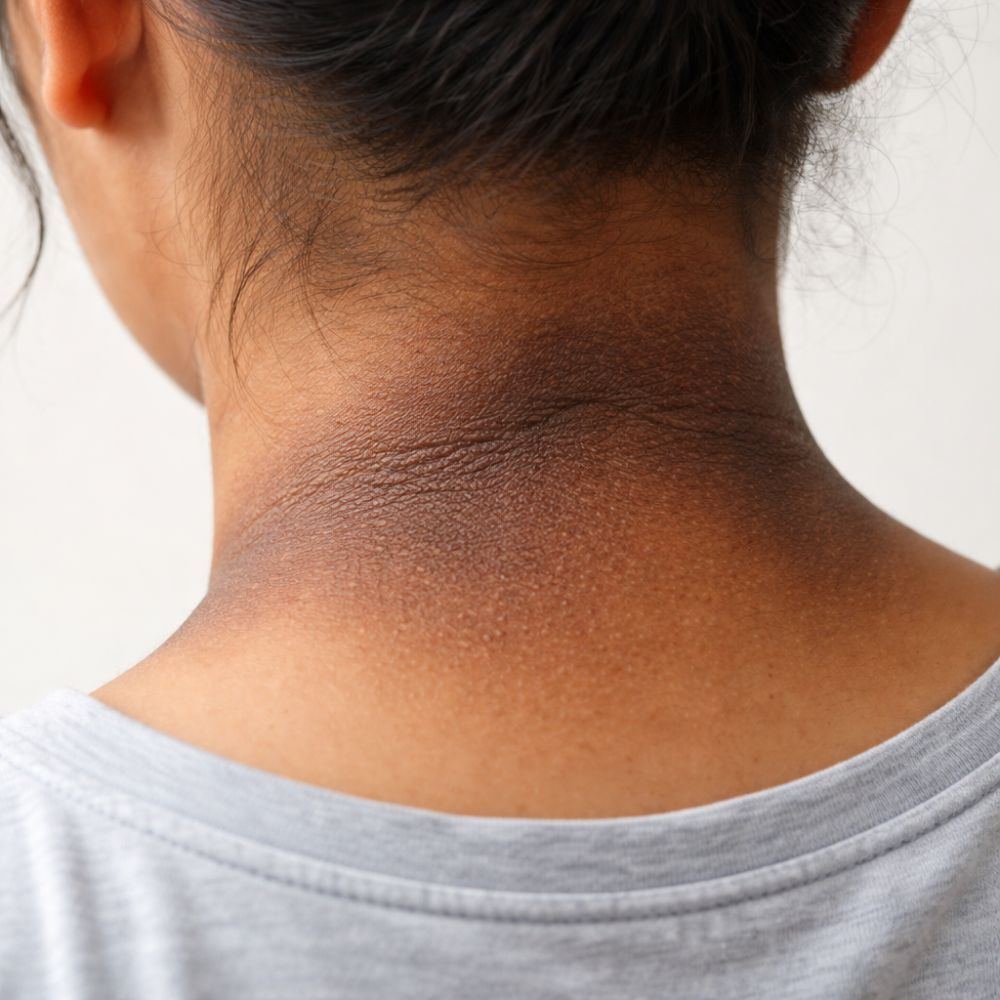
8. Skin Changes (Acanthosis Nigricans): A common skin manifestation of insulin resistance is the appearance of dark, velvety patches of skin, typically in body folds and creases like the neck, armpits, or groin. This condition, called acanthosis nigricans, is a strong indicator that the body is producing excess insulin in an attempt to overcome cellular resistance.
9. Irritability and Mood Changes: The brain requires a steady supply of glucose to function properly. Wild swings in blood sugar levels can affect brain function and mood. When blood sugar is high, you might feel fatigued and irritable. When it drops too low (which can happen as the body overproduces insulin), you can feel anxious, shaky, and confused. These fluctuations can lead to uncharacteristic moodiness and a short temper.
Why are These Diabetes Symptoms Considered Hidden?
These diabetes symptoms are considered hidden because they are often nonspecific, develop slowly over months or even years, and can be easily attributed to other common life factors such as aging, stress, fatigue, or minor illnesses.
Unlike the classic symptoms of excessive thirst (polydipsia) and frequent urination (polyuria), which are more dramatic and harder to ignore, these subtler signs do not immediately scream diabetes. This subtlety is what makes them so dangerous, as it allows the underlying condition to progress undiagnosed and untreated, potentially leading to significant health complications before it is ever identified.
For example, a person experiencing increased fatigue and irritability might blame it on a demanding job or lack of sleep. Someone with slow-healing sores might think they just have a minor skin issue or are not taking proper care of a wound. Recurring yeast infections are often treated as isolated gynecological or dermatological problems without considering a systemic cause.
Similarly, blurred vision might be dismissed as a sign of needing new glasses, and unexplained weight loss could even be initially welcomed before it becomes concerning. The gradual onset of these symptoms allows a person to adapt to them, normalizing what should be recognized as a significant change in their health.
This process of misattribution is a major barrier to early diagnosis, particularly in Type 2 diabetes, which accounts for the vast majority of cases and typically has a much slower, more insidious onset than Type 1 diabetes.
Because these signs are not definitive on their own, people and even healthcare providers might not connect the dots to suspect an underlying metabolic disorder until the symptoms become more severe or a routine blood test reveals an abnormality.
What Causes These Hidden Diabetes Signs
These hidden diabetes symptoms are caused by the physiological damage resulting from persistently high levels of glucose in the bloodstream, a condition known as hyperglycemia. This state arises from either an absolute deficiency of insulin (as in Type 1 diabetes) or the body’s inability to use insulin effectively, known as insulin resistance (the hallmark of Type 2 diabetes), which in turn damages nerves, blood vessels, and organs throughout the body.
Next, we will explore the specific mechanisms through which hyperglycemia gives rise to some of the most common hidden symptoms, such as nerve damage and vision problems.
High Blood Sugar Leads to Nerve and Vision Problems
High blood sugar leads to nerve and vision problems primarily by damaging the small blood vessels (microvasculature) that supply them with oxygen and nutrients, and by directly injuring the cells themselves through metabolic stress.
This dual-pronged attack slowly degrades the function of both the peripheral nervous system and the delicate structures of the eye, leading to conditions like diabetic neuropathy and retinopathy.
The process is gradual and often asymptomatic in its early stages, which is why these symptoms are considered “hidden” until the damage becomes significant enough to be noticeable.
In the case of nerve damage (neuropathy), hyperglycemia initiates a complex cascade of events. Excess glucose can be converted into other substances like sorbitol, which accumulates in nerve cells and causes them to swell and sustain damage.
Furthermore, high blood sugar impairs blood flow to the nerves by damaging the capillaries that nourish them. This reduced blood flow deprives the nerve fibers of essential oxygen and nutrients, leading to their progressive deterioration.
The longest nerves in the body, those extending to the feet and hands, are typically affected first, resulting in the characteristic symptoms of tingling, burning pain, or numbness that begin in the toes and fingers and can gradually spread upwards. For vision problems, the mechanism is similar.
In the short term, high blood glucose can cause the lens of the eye to swell, altering its curvature and refractive power, which results in blurred vision. This is often reversible once blood sugar levels are brought under control. However, chronic hyperglycemia inflicts long-term, irreversible damage on the retina. The tiny blood vessels in the retina can become blocked, leak fluid, or grow abnormally in a condition called diabetic retinopathy.
This process can lead to macular edema (swelling in the central part of the retina), retinal detachment, and eventually, permanent vision loss if not managed through strict glucose control and specialized ophthalmological treatments.
The Causes of Symptoms in Type 1 and Type 2 Diabetes
While the hidden symptoms of diabetes are nearly identical for both Type 1 and Type 2, the root causes of the underlying hyperglycemia are fundamentally different. The primary distinction lies in the origin of the insulin problem: Type 1 diabetes is characterized by an absolute lack of insulin due to autoimmune destruction, whereas Type 2 diabetes begins with insulin resistance, where the body’s cells fail to respond to the hormone properly.
Despite these different starting points, both paths converge on the same result: an excess of glucose in the bloodstream that wreaks havoc on the body’s systems.
In Type 1 diabetes, the body’s own immune system mistakenly attacks and destroys the insulin-producing beta cells in the pancreas. This is an autoimmune condition, and the result is a complete or near-complete inability to produce insulin.
Without insulin to act as a key, glucose cannot enter the body’s cells to be used for energy and instead accumulates in the blood. The onset of symptoms in Type 1 is often rapid and severe, occurring over weeks or months, and can include dramatic weight loss as the body breaks down muscle and fat for fuel in a state of cellular starvation.
In contrast, Type 2 diabetes, which accounts for about 90-95% of all diabetes cases, develops much more slowly. It begins with insulin resistance, a condition where muscle, fat, and liver cells do not use insulin efficiently. Initially, the pancreas compensates by producing more and more insulin to overcome this resistance.
However, over time, the beta cells can become exhausted and can no longer keep up with the high demand, leading to a relative insulin deficiency and rising blood glucose levels. The symptoms of Type 2 diabetes are often subtle and develop over many years, which is why many individuals are unaware they have the condition until complications arise.
Therefore, while a Type 1 patient’s symptoms are caused by an absence of insulin, a Type 2 patient’s symptoms are caused by the body’s failed response to it, but the end-stage physiological damage from high glucose is the same.
When to Consult A Healthcare Professional
You should absolutely see a doctor if you experience any of these hidden signs of diabetes, especially if you notice several of them occurring simultaneously or if you have other risk factors for the disease. These symptoms are your body’s way of signaling that its ability to regulate blood sugar is compromised, and ignoring them can allow for the progression of the disease and the development of severe, irreversible health complications.
While it may be tempting to dismiss signs like fatigue, frequent infections, or blurred vision as minor issues or consequences of a busy lifestyle, they can be indicators of a serious underlying metabolic condition. Self-diagnosis or ignoring these symptoms is dangerous because uncontrolled diabetes can cause progressive and silent damage to your heart, kidneys, nerves, and eyes.
Only a qualified doctor can perform the necessary tests to determine if your symptoms are related to diabetes or another medical issue. First, early diagnosis and intervention are the cornerstones of effective diabetes management.
The sooner you are diagnosed, the sooner you can implement lifestyle changes, such as diet and exercise, and, if necessary, begin medication to control your blood glucose levels. This proactive approach is proven to significantly reduce the risk of long-term complications like heart attack, stroke, kidney failure, and amputations.
Second, many of the hidden symptoms of diabetes are non-specific and can overlap with other conditions. A healthcare professional can conduct a thorough evaluation, review your medical history, assess your risk factors (such as family history, obesity, and age), and order the appropriate diagnostic tests to provide an accurate diagnosis. Attempting to manage the situation on your own without a clear understanding of the cause could lead to ineffective or even harmful actions.
Finally, a diabetes diagnosis is not just a label; it is the beginning of a partnership with your healthcare team to create a personalized management plan that works for you. This plan will empower you with the knowledge and tools needed to live a long and healthy life with the condition.
What Diagnostic Tests Are Used to Confirm Diabetes?
There are three primary blood tests used to confirm a diagnosis of diabetes or prediabetes: the Hemoglobin A1c (A1C) test, the Fasting Plasma Glucose (FPG) test, and the Oral Glucose Tolerance Test (OGTT).
Each test measures blood glucose levels in a different way, and sometimes a doctor may use a combination of tests or repeat a test on a different day to confirm the diagnosis, ensuring accuracy before initiating a treatment plan.
- Hemoglobin A1c (A1C) Test:
This is a common and convenient blood test that provides an estimate of your average blood glucose levels over the preceding two to three months. It measures the percentage of hemoglobin, the protein in red blood cells that carries oxygen, that is coated with sugar (glycated). A higher A1C percentage corresponds to higher average blood sugar levels.
For diagnosis, an A1C level of 6.5% or higher indicates diabetes. A level between 5.7% and 6.4% suggests prediabetes, while a result below 5.7% is considered normal. This test does not require fasting.
- Fasting Plasma Glucose (FPG) Test:
This test measures your blood glucose level at a single point in time after you have fasted (not eaten or drunk anything except water) for at least eight hours. It is typically performed in the morning.
A fasting blood glucose level of 126 milligrams per deciliter (mg/dL) or higher on two separate occasions indicates diabetes. A result between 100 and 125 mg/dL is classified as prediabetes (also known as impaired fasting glucose), and a level of 99 mg/dL or below is normal.
- Oral Glucose Tolerance Test (OGTT):
The OGTT is a more sensitive test that assesses how your body processes glucose over time. It requires you to fast overnight and then have your blood drawn to establish a baseline fasting glucose level. Afterward, you drink a standardized sugary liquid, and your blood glucose level is tested again two hours later. A blood glucose level of 200 mg/dL or higher after two hours indicates diabetes.
A result between 140 and 199 mg/dL indicates prediabetes (also called impaired glucose tolerance), and a reading below 140 mg/dL is considered normal. This test is frequently used to diagnose gestational diabetes in pregnant women.
Broader Health Implications Of Diabetes
The broader health implications of diabetes extend far beyond managing blood sugar, involving long-term risks to cardiovascular, nervous, and renal systems, while management strategies focus on lifestyle modifications, medication, and regular monitoring to prevent complications.
Furthermore, understanding the precursor stage of prediabetes, identifying personal risk factors, and distinguishing diabetes from conditions with similar symptoms are crucial for both effective prevention and accurate diagnosis. A comprehensive approach involves not just treating high blood glucose but also addressing the interconnected physiological systems that diabetes affects over time.
How Does Prediabetes Differ From Full-Blown Diabetes?
Prediabetes is a critical warning stage where blood glucose levels are elevated but have not yet crossed the threshold for a Type 2 diabetes diagnosis; it signifies a high risk of future disease development but also presents a crucial opportunity for prevention through intervention.
The primary distinction lies in the diagnostic criteria: a fasting plasma glucose level between 100-125 mg/dL indicates prediabetes, while a level of 126 mg/dL or higher signifies diabetes. Similarly, an A1c level between 5.7% and 6.4% is classified as prediabetes, whereas 6.5% or higher confirms diabetes.
Unlike full-blown diabetes, which is a chronic, progressive condition often requiring lifelong medication and management, prediabetes is frequently reversible. While individuals with Type 2 diabetes often experience noticeable symptoms like increased thirst, frequent urination, and fatigue, prediabetes is typically asymptomatic, making regular screening essential for those with risk factors.
The core difference is one of progression and reversibility; managing prediabetes aims to halt or reverse the progression to diabetes, whereas managing diabetes focuses on controlling the existing condition to prevent severe complications like heart disease, kidney failure, and nerve damage. This distinction underscores the importance of early detection and proactive management.
- Goal of Intervention: For prediabetes, the primary goal is prevention, to lower blood sugar levels back to the normal range and prevent the onset of Type 2 diabetes. For diagnosed diabetes, the goal is control, to manage blood glucose levels consistently to minimize the risk of acute and chronic complications.
- Symptom Presentation: Prediabetes rarely presents with overt symptoms, making it a silent condition. In contrast, Type 2 diabetes, while sometimes subtle, often manifests with the classic signs of hyperglycemia, including blurred vision, slow-healing sores, and unexplained weight loss.
- Pathophysiological State: In prediabetes, the body’s cells are beginning to show signs of insulin resistance, or the pancreas may not be producing enough insulin to keep up with demand. In full-blown Type 2 diabetes, this resistance is more pronounced, and the pancreas’s ability to produce insulin is significantly impaired.
The Primary Risk Factors for Developing Type 2 Diabetes
The development of Type 2 diabetes is influenced by a combination of non-modifiable and modifiable risk factors that contribute to insulin resistance and impaired insulin secretion. Understanding these factors is key to assessing personal risk and implementing preventive strategies.
Family history is a significant non-modifiable risk; having a parent or sibling with Type 2 diabetes substantially increases one’s own risk, pointing to a strong genetic predisposition. Age is another critical factor, with risk increasing significantly after the age of 45, likely due to a natural decline in pancreatic function and an increase in insulin resistance over time.
Ethnicity also plays a role, as certain populations, including African Americans, Hispanic/Latino Americans, American Indians, and Asian Americans, have a genetically higher risk. Modifiable risk factors, however, are largely tied to lifestyle. Overweight and obesity, particularly the accumulation of visceral fat around the abdomen, is the single most important predictor.
Excess adipose tissue promotes inflammation and releases substances that interfere with insulin signaling. Physical inactivity is another major contributor, as regular exercise helps control weight and improves insulin sensitivity, allowing cells to use glucose more effectively.
Identifying these risk factors allows for targeted lifestyle interventions.
- Weight and Body Composition: A Body Mass Index (BMI) of 25 or higher is a primary risk factor. The location of body fat is also crucial; a larger waist circumference is indicative of central obesity and a higher risk of insulin resistance compared to fat stored in the hips and thighs.
- Co-existing Medical Conditions: Certain health issues are closely linked to the development of Type 2 diabetes. These include high blood pressure (hypertension), low levels of high-density lipoprotein (HDL or “good”) cholesterol, high levels of triglycerides in the blood, and a history of gestational diabetes or Polycystic Ovary Syndrome (PCOS) in women.
- Dietary Habits: A diet high in processed foods, sugary beverages, and unhealthy fats, while low in fiber, fruits, and vegetables, contributes to weight gain and directly impacts blood sugar control, increasing the long-term risk of developing the disease.
The Symptoms Overlap Between Diabetes And Thyroid Disorders
Diabetes and thyroid disorders, particularly hypothyroidism and hyperthyroidism, share several overlapping symptoms because both conditions disrupt the body’s metabolism, albeit through different hormonal pathways. This symptomatic crossover can complicate initial diagnosis and underscores the need for precise medical testing.
Unexplained weight changes are a classic example: uncontrolled Type 1 or Type 2 diabetes can cause weight loss as the body burns fat and muscle for energy, while hyperthyroidism (an overactive thyroid) accelerates metabolism, also leading to weight loss.
Conversely, hypothyroidism (an underactive thyroid) slows metabolism, often causing weight gain, which is also a common risk factor for and symptom associated with developing Type 2 diabetes.
Fatigue and persistent lethargy are hallmark symptoms of both conditions. In diabetes, fatigue results from cells being unable to access glucose for energy, while in thyroid disorders, it stems from either an overly accelerated or slowed metabolic rate.
Mood swings, anxiety, and irritability are also common in both, linked to fluctuating blood sugar levels in diabetes and the direct impact of thyroid hormones on neurotransmitters in the brain. Other shared signs include changes in skin (dry skin in hypothyroidism and diabetes) and increased sensitivity to temperature.
A differential diagnosis based on specific blood tests is essential to distinguish between these conditions.
- Mechanism of Fatigue: In diabetes, fatigue is due to hyperglycemia or hypoglycemia, where cells are starved of or overwhelmed by glucose. In hypothyroidism, fatigue arises from a systemic slowing of all bodily processes, whereas in hyperthyroidism, it can be due to muscle weakness and sleep disruption from an overstimulated nervous system.
- Weight and Appetite Changes: Uncontrolled diabetes often presents with polyphagia (increased hunger) alongside weight loss. Hyperthyroidism also causes increased appetite but with weight loss. Hypothyroidism typically leads to weight gain despite a normal or reduced appetite.
- Cardiovascular Symptoms: Both conditions can affect the heart. Hyperthyroidism can cause a rapid or irregular heartbeat (tachycardia or palpitations), while diabetes contributes to long-term cardiovascular disease through mechanisms like high blood pressure and atherosclerosis.
How to Manage and Prevent Diabetes
Lifestyle changes centering on diet, physical activity, and weight management are the cornerstones of both preventing Type 2 diabetes and effectively managing all types of diabetes. These interventions work synergistically to improve insulin sensitivity, control blood glucose levels, and reduce cardiovascular risk factors.
A foundational dietary change is adopting a balanced eating pattern rich in whole, unprocessed foods. This involves prioritizing non-starchy vegetables, lean proteins, and healthy fats while moderating the intake of carbohydrates, especially refined ones.
Focusing on foods with a low glycemic index (GI), such as whole grains, legumes, and most fruits, helps prevent sharp spikes in blood sugar. Portion control is equally vital to manage calorie intake and support weight management. Regular physical activity is another critical pillar.
A combination of aerobic exercise (like brisk walking, swimming, or cycling) and strength training is ideal. Aerobic activity helps the body use insulin more efficiently, while strength training builds muscle mass, which increases the number of glucose receptors on cells, thereby improving glucose uptake from the bloodstream.
The American Diabetes Association recommends at least 150 minutes of moderate-intensity aerobic exercise per week, spread over several days. These lifestyle modifications are powerful tools for gaining control over the disease’s progression.
- Weight Management: For individuals who are overweight or obese, even modest weight loss can have a profound impact. Losing just 5-7% of total body weight has been shown to significantly delay the onset of Type 2 diabetes in high-risk individuals and improve glycemic control in those already diagnosed.
- Consistent Meal Timing: Eating meals and snacks at regular intervals throughout the day can help maintain stable blood sugar levels and prevent extreme fluctuations. Skipping meals can lead to hypoglycemia, while large, infrequent meals can cause significant spikes.
- Stress Reduction and Adequate Sleep: Chronic stress can raise blood sugar levels through the release of cortisol, and poor sleep has been linked to impaired insulin sensitivity. Incorporating stress-management techniques like mindfulness or yoga and aiming for 7-9 hours of quality sleep per night are important complementary strategies for diabetes management.
FAQs
How do I know if I have diabetes without testing?
You cannot confirm diabetes without medical testing. Symptoms can guide your awareness, but only blood tests such as fasting glucose or HbA1c can provide a clear diagnosis. If several signs of diabetes are present, testing becomes essential.
How to know if you have diabetes or just temporary symptoms?
Temporary symptoms usually resolve within a few days. Diabetes-related symptoms tend to persist or gradually worsen over weeks or months. If patterns continue, medical evaluation is necessary.
What are the most common signs of diabetes in men?
Signs of diabetes in men can include fatigue, unexplained weight loss, reduced physical endurance, and sometimes changes in sexual health. These often appear alongside more general symptoms like thirst and frequent urination.
Can you have diabetes without noticeable symptoms?
Yes, especially in type 2 diabetes. Some individuals experience very mild symptoms or none at all in the early stages. This is why routine health screenings are important, even when you feel normal.
How long can diabetes go unnoticed?
Diabetes, particularly type 2, can go undiagnosed for years. During this time, damage to blood vessels, nerves, and organs may already begin. Early recognition of signs and symptoms of diabetes can prevent long-term complications.
Can lifestyle changes reverse early diabetes signs?
In many cases, early intervention through diet, physical activity, and weight management can significantly improve blood sugar control. While not all cases are reversible, early changes can delay or prevent progression.
Conclusion
Your body communicates through patterns, not just isolated symptoms. When you start asking how do I know if I have diabetes, that question itself is already a signal worth paying attention to.
Awareness is the first step toward control, and early action can change the entire trajectory of your health.
References:
- International Diabetes Federation – Over 250 million people worldwide unaware they have diabetes
- American Diabetes Association – Sex and Diabetes
- CDC – Diabetes and Your Skin
Disclaimer
This article is intended for informational and educational purposes only. We are not medical professionals, and this content does not replace professional medical advice, diagnosis, or treatment.
The goal is to provide accurate, evidence-based information to raise awareness of signs of diabetes and related conditions. If you are experiencing persistent, severe, or concerning symptoms, you should seek guidance from a qualified healthcare provider.
Read more: 12 Foods and Drinks Diabetics Need to Avoid